Before You Come To The Hospital
• Important Phone Numbers
• Schedule of Follow-up visits
• A Closer Look at Total Hip Replacement
Your Surgery and Hospital Stay
• The Day of the Surgery
• Recovering in the Hospital
• Managing Pain
• Rehabilitation in the Hospital
• Do's and Don'ts in the Hospital
• Preventing Blood Clots
• Diet
• Preparing to Return Home
Final Steps: At Home
• Guidelines for Home Recovery
• Preventing Infection
• Sports Activities
• Do's and Don'ts During Home Recovery
• Sexual Relations
• Home Recovery Program
• Home Recovery Exercise Program
• Advanced Exercises
Important Telephone Numbers
Ortho Excel - 9920053334
Other Important Numbers http://www.orthoexcel.in/contacts.htm
Schedule of Follow-Up visits
Expect to have routine follow-up visits at the Ortho Excel as follows:
• Suture removal 10-14 days from surgery
• 6 weeks following day of surgery
• 3 months following total hip replacement
• 1 year following total hip replacement
• 3 years following total hip replacement
• 5-6 years following total hip replacement
• 8-10 years following total hip replacement
This follow-up schedule may vary from patient to patient. You must call the Ortho Excel Staff to schedule all appointments. Please notify us if you have a change of name, address, telephone number or insurance carrier.
A Closer Look at Total Hip Replacement
To understandtotal hip replacement, you should be familiar with the structure of the hip joint, a ball-and-socket joint. The ball component is attached to the top of the femur (long bone of the thigh). The socket is part of the pelvis. The ball rotating in the socket permits you to move your leg forward, backward and sideways, i.e. in all planes of motion.
|
|
|
|
| With a healthy hip, smooth cartilage covering the ends of the thigh bone and pelvis allows the ball to glide easily inside the socket. |
|
With a problem hip, the worn cartilage no longer serves as a cushion. As the diseased or damaged bones rub together, they become rough, and the resulting pain causes difficulty in walking. |
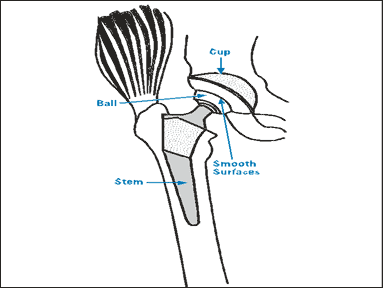
Total Hip Replacement consists of replacing the worn out socket with a durable plastic or polyethylene cup with or without a metal titanium shell. The ball is replaced with a chromium-cobalt alloy metal ball that is attached to a metal stem of titanium or chromium cobalt metal alloy.
There are several ways to fasten the components during the hip replacement procedure (implant to the bone). With a cemented total hip replacement, the prosthesis is held in place by bone cement. In a non-cemented total hip replacement, fixation occurs as the bone grows on and into the implant surface. With a hybrid total hip replacement, the femoral component in the thigh bone is cemented, and the acetabular component is affixed by bone growing on and into the implant surface, which consists of a titanium or cobalt chromium shell and a polyethylene liner.
Bearing surfaces include metal-on-polyethylene, ceramic-on-ceramic and metal-on-metal. The most commonly used FDA approved bearing surface is metal with highly cross-linked polyethylene. The best bearing surface for you will be decided in consultation with your surgeon.
Clinical and biomechanical research has steadily improved the methods and materials available for total hip replacement. Prosthesis durability varies with the usage demands of each patient.
Before You Come to The Hospital
Total Hip Replacement can enhance your quality of life by providing many years of improved mobility and reduced pain. Each year over 200,000 Americans benefit from Total Hip Replacement.
In the last decade remarkable improvements in technology have transformed total hip replacement into an efficient and widely performed procedure.
Dr. Rahul Shah, M.D. and his associates are supported by a large staff of fellows, residents, physician assistants, anesthesiologists, physical therapists, social workers and administrative personnel.
A Checklist of Things To Do
• You may be asked to donate your blood for the surgery. If the donation is required, the Ortho Excel staff will make an appointment for you at the Hospital's Blood Donor Center.
• Our staff will make an appointment for you for pre-surgical testing fourteen (14) days prior to surgery.
• Our Staff will make an appointment for your examination with an internist at the Hospital before your surgery. The internist will:
- Review and/or perform any necessary diagnostic tests
- Provide medical clearance for the surgical procedure
• Unless you are told otherwise, continue to take medicines already prescribed by your own physician. Also anti-inflammatory medications and anti-oxidant vitamins such as C and E should be discontinued ten (10) days prior to your Admission.
DO NOT EAT OR DRINK ANYTHING AFTER MIDNIGHT ON THE NIGHT BEFORE YOUR SCHEDULED SURGERY, UNLESS OTHERWISE INSTRUCTED.
Recovering in the Hospital
After surgery, your IV (intravenous) line will remain in your arm for approximately 48 hours. The IV line delivers fluids, antibiotics and other medications. Should you need a blood transfusion, the IV line can also deliver blood.
The surgical site will be bandaged. A thin tube inserted into the site and attached to a drain prevents blood from accumulating around the hip. This tube is removed the day after surgery and the bandage is removed the second post-surgical day.
A pillow between your legs will help maintain the proper position of your hip. A nurse will position you in bed and help you turn until you are able to move on your own.
Because anesthesia may temporarily inhibit urination after surgery, a catheter may be inserted into the bladder to remove urine. When the patient regains function, usually within one to two days after surgery, this catheter is removed.
In collaboration with you and your family, the hospital staff, including a physician, physician assistant, nurse, physical therapist, and social worker will plan, provide and monitor your care.
Exercise
Gentle exercise to improve your range of motion can help prevent circulation problems as well as strengthen your muscles. As soon as you are able after surgery, a physical therapist will teach you the necessary exercises.
Deep Breathing
After surgery, regular deep breathing, to rid your air passages of mucus, is vitally important. Normally, you take deep breaths almost every hour, usually without being aware of it, whenever you sigh or yawn. When you are in pain, or are drowsy from anesthesia or pain medication, your breathing may be shallow.
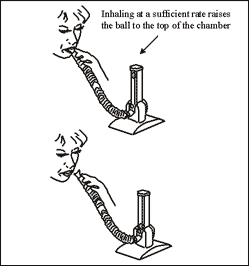
To ensure that you breathe deep daily, the nursing staff will provide you with a device called an Incentive Spirometer, along with instructions on its use. |
|
 |
| |
|
|
How to use the Incentive Spirometer
With the unit in an upright position, place your lips tightly around the mouth-piece and exhale normally.
To achieve a deep and sustained breath, inhale at a rate sufficient to raise the ball in the chamber.
Exhale. After performing the exercise, remove the mouthpiece from your lips.
Relax and breathe normally for a moment after each deep breath.
Repeat this exercise 10 times every hour.
Managing Pain
How does it feel?
Recovering from any surgery involves pain and discomfort. The hospital's team approach to pain management can help reduce your discomfort and thus speed your recovery.
Pain management, however, begins with you. Since there are no objective tests to measure what you are feeling, you must help the staff by describing the pain, pinpointing its location, and judging its intensity, as well as reporting any changes in these. Sometimes pain is constant. Other times it is sporadic. It can be sharp, burning, tingling or aching.
The Pain Scale
Worst Pain No Pain
10 9 8 7 6 5 4 3 2 1
• • • • • • • • • • • • • • •
Always report any increases or changes in pain. As we discuss below, there are several approaches to pain relief. To fully reap their benefits, you must use them before pain becomes severe.
Pain management will be decided by the surgeon and the surgical team. The main methods of pain control after surgery include:
• Approach 1: Epidural Anesthesia
Epidural anesthesia, for one to two days post-surgery, will keep your pain at a low level on the pain scale. However, after the epidural is discontinued, your pain can be managed by oral or injectable medication. An epidural pump and a PCA pump look similar.
• Approach 2: Patient Controlled Anesthesia (PCA)
Patient controlled anesthesia (PCA) will be provided if requested, or if the epidural wears off or is stopped for medical reasons.
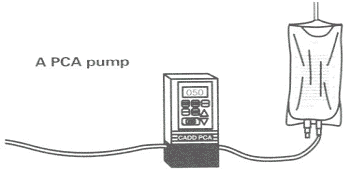
• Approach 3: Oral Medication
Approximately 24 to 48 hours after surgery, as pain decreases, you will begin to increase your activity, at which time you will switch to oral or injectable pain medications, which control discomfort and do not restrict activity or mobility.
Cold Therapy
During your hospital stay, ice packs applied to the surgical site by the nursing staff while you are at bed-rest, will aid in reducing swelling and pain.
All pain medications are carefully prepared by hospital pharmacists to assure quality and safety. Medications used include Fentanyl and Morphine, which are narcotics, and Bupivacaine, also known as Marcaine, which is a local anesthetic.
PLEASE INFORM THE ANESTHESIOLOGIST OF ANY PREVIOUS UNUSUAL REACTIONS TO PAIN MEDICATION. THIS INFORMATION SHOULD ALSO BE INCLUDED IN THE MEDICAL INFORMATION YOU BRING TO THE HOSPITAL.
Rehabilitation in the Hospital
Your participation in a physical therapy program is essential to the success of your surgery. The more committed and enthusiastic you are, the speedier your improvement will be.
The day after surgery, a physical therapist will visit you with an exercise program to increase your hip's range of motion and strengthen your leg muscles. In the first few days after surgery, you may benefit from taking pain medication one hour prior to your physical therapy session. Check with your nurse and/or therapist. Also, the therapist will review necessary precautions to prevent hip dislocation.
The physical therapist will assist you in the following activities:
• Sitting at bedside with your legs dangling
• Standing with the aid of a walker
• Climbing stairs
• Arranging attendance to Activities of Daily Living Class, where you will learn how to live and thrive with your total hip replacement.
Before leaving the hospital, most patients progress to forearm crutches and can get in and out of bed unassisted.
Do's and Don'ts After Your Total Hip Replacement
Below is a general list of precautions to follow after your total hip replacement. If additional precautions are necessary, the staff will provide instructions.
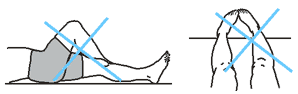
Lying Down
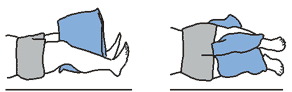
• Keep the abductor pillow between your knees when you lie on your back.
• Keep the bed flat when you exercise or get out of bed.
• You may turn on the non-operated side with the help of your nurse.
• Avoid crossing your legs.
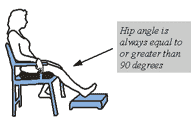
Sitting
Your surgeon or therapist will tell you when to start sitting in a high chair.
Do:
• Keep your knees lower than or equal to your hips.
• Use a high toilet or a raised toilet seat on a standard toilet.
• Sit on a firm chair (preferably) using two firm pillows.
|
|
 |
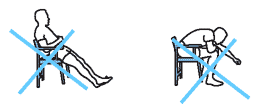
Don't:
• Sit in low, soft chairs such as sofas.
• Bend to pick up any objects from the floor.
• Bend to clean or dry your feet.
|
|
If you leave the hospital by carpenter the car from street level to avoid bending your hip too far; sit in the front seat, making sure the car seat is all the way back and in an upright position. Sit on two pillows.
Showering
You may take a shower only after sutures have been removed. Also, use a grab bar or shower chair for added safety, comfort and stability.
• Don't take a tub bath.
Sutures
Sutures should be removed 10 to 14 days following surgery. Please call the Ortho Excel at (646) 797-8700 for an appointment or they can be removed by VNS.
Preventing Blood Clots
After total hip replacement surgery, clots, called deep vein thromboses (DVT), may form in the leg veins. In rare cases, these leg clots travel to the lung, where they may cause symptoms. To prevent and reduce the incidence of clot formation, mechanical devices are used to squeeze the leg muscle, thus maintaining blood flow in the veins. Also, a medication to minimize clot formation, such as Coumadin, Heparin, Aspirin or Persantine, is prescribed.
Ultrasound Doppler
Before your discharge from the hospital, you will receive a noninvasive test to detect blood clots. The test relies on sound waves generated by moving blood cells. You will be asked to lie in a semi-upright position. The procedure causes no discomfort, and no special preparation is required. If no clots are found, you will be discharged on Aspirin 325 mg a day for one (1) month. If your doppler results are positive, your surgeon will determine the necessary treatment.
Leg Swelling
Following hip replacement, most patients develop swelling in the operated leg. Although the amount of swelling can vary from patient to patient, the swelling itself in the leg, knee, ankle or foot is normal, and will usually resolve gradually over several weeks.
For the first month after your operation, the amount of time spent in a sitting position should be 30 TO 45 MINUTES ONLY, as sitting tends to worsen the swelling. Periods of walking should be alternated with periods of elevating the swollen leg. When elevating the leg, the ankle should be above the level of the heart. You should lie with one pillow under your head and four to five pillows under your foot and leg to elevate your leg above your chest.
DO NOT ELEVATE YOUR FEET while sitting in a chair.
It is often helpful to spend an hour in this elevated position in the early afternoon to help diminish the swelling which may have developed during your morning walks.
To prevent or reduce leg and ankle swelling:
• Elevate the operated leg
• Avoid sitting for more than 30 to 45 minutes at a time
• Perform ankle exercises
• Use elastic compression socks
Diet
During your hospital stay, eat balanced, nutritious meals with adequate calories and protein to enable your body to replenish proteins depleted by surgery, and to reduce the risk of complications such as infection or poor wound healing. Being adequately nourished is an important component of your overall health and promotes your recovery.
After surgery, most patients will be placed on a liquid diet for 3 or 4 days, as appetite may be poor and the effect of anesthesia on intestinal function can last a few days. We encourage you to eat only when you feel hungry, to prevent nausea. Not having a bowel movement for 4 to 5 days following surgery is normal.
FINAL STEPS: AT HOME
Caring for Surgical Site
1. Leave the Primapore Dressing on if drainage occurs, if not take of the dressing and leave the wound open to air.
2. After removal of your sutures, leave the incision open unless instructed otherwise.
3. Please inform ROC of increasing redness of or drainage from your incision.
Pain Medication
1. Take your pain medication as prescribed.
2. To control pain, take your pain medication before the pain becomes severe.
3. If your pain medication seems weak, or if you are experiencing unpleasant side effects, do not hesitate to call the Ortho Excel.
4. If you are taking pain medication, avoid alcoholic beverages and recreational drugs.
5. If you experience discomfort during your ongoing physical therapy, take your pain medication at least 45 minutes prior your subsequent therapy sessions to allow enough time for the medication to take effect.
Preventing Infection
Having undergone surgery increases your risk of infection. However, antibiotics can help protect you and should be used in the following situations:
• With any medical or surgical procedure, performed by your physician or dentist.
• During certain diagnostic procedures, such as catheterization and endoscopy, or those involving intestines, lungs, bladder and kidney.
• With serious infections elsewhere in your body.
Tell your internist and dentist that you have an artificial joint so that they can prescribe antibiotics. If you have questions or concerns, please call us.
Total hip replacement patients who require dental work on gums or roots must adhere to the following antibiotic procedure:
For patients not allergic to Penicillin: Cephalexin, Cephradine or Amoxicilin: 2 grams orally 1 hour prior to the dental procedure
For patients allergic to Penicillin: Clindamycin: 600mg orally 1 hour prior to the dental procedure.
Patients should adhere to this regimen for the first two years following joint replacement. Immunocompromised patients, including those with inflammatory arthropathies, rheumatoid arthritis, drug or radiation-induced immunosuppression, insulin-dependent diabetes or any other major medical problem should follow this antibiotic routine indefinitely.
Antibiotics can reduce the risk of infection but cannot completely eliminate that risk. Preventing infection must be the concern of all the healthcare professionals who treat you. MAKE SURE YOU INFORM YOUR PHYSICIAN AND DENTIST THAT YOU HAVE HAD A TOTAL HIP REPLACEMENT.
Sports Activities
After full recovery, some patients enjoy light sports activities. Activities you can enjoy after total hip replacement include walking, bicycling, bowling, swimming, golf and doubles tennis. Avoid high impact activities, such as:
• Jogging
• Running
• Jumping
• Skiing
Do's and Don'ts During Home Recovery
Precautions for home recovery are, with slight modification, the same as those you followed in the hospital. However, based upon various factors such as health history, type of implant, etc., your physician or physical therapist may give you additional guidelines.
Lying Down
Do:
• Keep the abductor pillow between your knees when you lie on your back. Keep the bed flat when you exercise or get out of bed.
• Turn on the non-operated side with the abductor pillow between your knees. Avoid crossing your legs.

Don't:
• Raise the head of your bed more than half upright (45 degrees) Lie on your operated side
• Cross your legs Roll your legs inward; your feet should be pointed up or outward

Sitting
Do:
• Keep your knees lower than or equal to your hips.
• Sit on a firm chair (preferably with arms) using two pillows.
• Use a high toilet or a raised toilet seat on a standard toilet.
When traveling by car:
• Enter from street level to avoid bending your hip too far.
• Sit on a firm cushion or pillow with the seat in an upright position as far back as possible.
Don't:
• Sit in low, soft chairs such as sofas.
• Bend to pick up any objects from the floor.
• Bend to clean or dry your feet.
Other positions to avoid following Total Hip Replacement
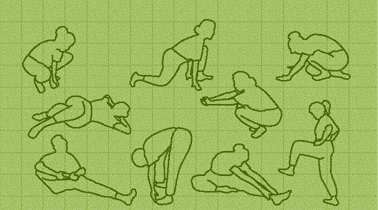
Sexual Relations
The following questions, answers and illustrations respond to the common concerns of patients and their partners after hip replacement surgery.
Will I be able to resume sexual relations now that my hip has been replaced?
The vast majority of patients are able to resume safe and enjoyable sexual intercourse after hip replacement. Patients whose sexual function had been impaired by preoperative hip pain and stiffness welcome their new pain-free mobility. However, gaining full confidence with your new hip may take several weeks.
When can I resume sexual intercourse?
In general, intercourse can be resumed safely approximately eight weeks after surgery. Though individual recovery time varies greatly, this timeframe allows the incision and the muscles around the hip to heal. If you recuperate rapidly, you will be able to resume sooner, as long as you are free of pain.
What positions are safe during intercourse?
Total hip replacement precautions need to be observed during all activities, including sexual intercourse. In general, follow the do's and don'ts on pages 26-27 and the positions illustrated on page 29. As advised in the discharge instructions, you should avoid excessive hip flexion (knee toward chest), adduction (leg towards center of body), and internal rotation (toes turned inward).
Most patients, male and female, prefer 'passive' intercourse in the 'bottom' position, an option some find less fatiguing. As your hip heals, you may resume a more active role. After a few months, patients can resume sexual activities in any comfortable position.
What should I tell my partner?
As good communication is essential, you may want to share information in this booklet with your partner. In addition, you can discuss the hip precautions that the hospital staff reviewed with you.
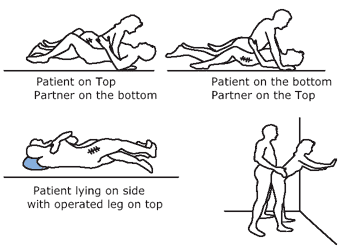
Sexual Positions Recommended Following Total Hip Replacement
Pillows placed under your knees can provide extra support and comfort
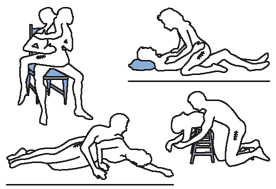
Sexual Positions to avoid Following Total Hip Replacement
Climbing Stairs
The following are instructions (NOT exercises) for climbing and descending stairs.
If you have one (1) total hip:
UPSTAIRS
• The non-operated leg goes first.
• The operated leg goes second.
• The crutches go last (at the same time as the operated leg).
DOWNSTAIRS
• The crutches go first.
• The operated leg goes second.
• The non-operated leg goes last.
If you have two (2) total hips:
UPSTAIRS
• The stronger leg goes first.
• The weaker leg goes second.
• The crutches go last(at the same time as the weaker leg).
DOWNSTAIRS
• The crutches go first.
• The weaker leg goes second.
• The stronger leg goes last.
Home Recovery Exercise Program
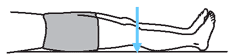
| Quad Set
Lying on your back:
1. Tighten thigh muscles by pressing knees down into the bed.
2. Hold for a count of 6. Do not hold your breath.
3. Relax.
4. Repeat. |
|
 |
| |
|
|
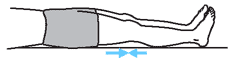
| Gluteal Set
Lying on your back:
1. Squeeze buttocks together.
2. Hold for a count of 6. Do not hold your breath.
3. Relax
4. Repeat
|
|
 |
| |
|
|
| Ankle Pumps
Lying on your back:
Keeping legs flat on bed, move both your ankles up and down.
|
|
 |
| |
|
|
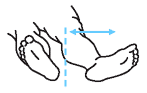
| Leg Rotation
Lying on your back:
1. Roll your operated leg inward so that your kneecap and foot are pointed toward the ceiling. Do not internally rotate your operated leg past this neutral point.
2. Relax
3. Repeat |
|
 |
| |
|
|
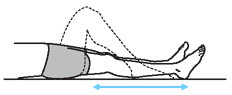
| Heel Slides
Lying on your back:
1. Bend hip and knee of operated side to about 40-45 degrees.
2. Hold for a count of 6. Do not hold your breath.
3. Relax
4. Repeat |
|
 |
| |
|
|
Advanced Exercises
These exercises place slightly greater demands on your hip. Progress to them only after you are seen by your surgeon on your first post-op visit.
| Straight Leg Raise
To build muscle strength perform this exercise twice each day. Work up to 20 lifts each time.
Lying on your back with your non-operated leg bent and your foot flat on the bed:
1. Raise your operated leg 12-18 inches.
2. Hold for 2 counts
3. Lower leg slowly.
4. Repeat
|
|
|
| |
|
|
| Side Leg Raise
To improve your hip's range of motion, perform this exercise twice each day. Work up to 20 lifts each time.
Lying on your non-operated side
1. Raise your operated leg 12-18 inches
2. Hold for 2 counts.
3. Lower leg slowly.
4. Repeat
|
|
 |
Stationary Bicycle
If you have a stationary bicycle, use it at no resistance for 15-20 minutes each day.
Swimming
Swim as much as you like. It is an excellent exercise and will help in your recovery. |